Death Nurse
Because this is a blog about living and dying, and because I'm a nurse.
Wednesday, May 15, 2024
Friday, January 19, 2024
Dr G and Me - Together Again! How to find your best option for hospice - Part 2, The Demo-ing
You can do it - you absolutely can in 5 simple steps
Dr G and Me - Together Again! How to find your best option for hospice - Part 1 of 2
How do you even start? Here's how
Monday, August 14, 2023
See me on TV with Dr G!
"That's me in the spot-light... trying to keep up with you"
(REM - 'Losing my Religion')
I'm grateful to Dr G for the chance to talk about what it was like trying to keep up with Jeanne
See more by Kaishauna Guidry,MD,HMDC and Mourning Dove Medical
Here are a few related posts about Jeanne
- A Death I Nursed
- David Bowie is helping me grieve
- Unconditional love
- Remembering Jeanne today
- Ice Cream, a Love Story
- Things that went badly... Part 1
- Things that went badly... Part 2
- Options for the final disposition of a dead body
- Understanding Alzheimer's - decline and prognosis
- I remember the day
- Death Nurse Film Fest V-1.2 (2019) - Ice Cream, a Love Story
- Life on Mars?
- Jeanne M. Soucy
Tuesday, April 11, 2023
New! Update for Updated Update: Game Over Updated
Four white dudes doing what they do
I returned to The Ira and VITAS! Show today for the first time since the 6th, and managed to follow along for another four (4!) of the episode's fifty-one (51!) minutes
Here's what I said in the comments this time...
OK so today I could handle about 4 minutes
I got re-oriented with Ira tossing out some nightmare clinical scenarios like bowel infarct, seizures and status epilepticus, though he didn't mention my personal favorite - massive sudden arterial bleed for tumor and tissue damage in head and neck cancer (dark towels?) - to emphasize the need for hospices to provide crisis levels of care (via continuous care in the home or general inpatient care at a licensed staffed facility)
Sure absolutely the IDT has to be prepared for the worst - part of every plan of care should be to ask: what's the worst that could happen? Then make sure to assess monitor prevent and intervene if needed because you were prepared
Now THAT's a great quality indicator
OK, now Ira's jabbering about "kind of have our hair on fire" - kind of? - then goes on to point out the many lost opportunities and failures by the professional orgs (oops) to do anything as it all happened under your nose and under your watch [ref above Christian admitting y'all haven't don't squat about it for 20 years]
I need to be honest with you here: you've been captured, the war is over and VITAS! dude's side won it all
Seriously, consider yourselves captives owned by the financial rapscallions who have taken over hospice, and they're just getting started, so really from here on out your jobs are all about harm reduction and keeping your heads down in order to survive in the current environment
Also too the orgs AAHPM RacistHPNA, of course the trade groups most notably NHPCO and org of orgs NCHPC (Ginger's new gig), etc - they're not just responsible for lots of the problems we're all in, but now also central to whatever "solutions" creep out of this mess or more specifically exploit it
Consider their whacky idea that one indicator of quality should be the number of nurses on staff who are certified CHPN etc via RacistHPNA - which is an excellent idea for RacistHPNA because dues + certification test prep and testing are pretty much the main revenue channels for orgs like RacistHPNA that still follow the model
I'm sure AAHPM is making that same play because orgs are platforms for commerce and careers and that's it
So, to repeat the obvious - you've lost everything at what''s likely the biggest board game most of you have ever played - your battleships are sunk, your king is surrounded etc etc etc
Your jobs are now harm reduction and keeping your head down in order to survive in the current environment
So Lauren has her hair on fire because there's no reason for 1,000 hospices in LA County (Ira says 800 so of course he does), then there's some chuckling about scammers and inside info because VITAS! dude knows where they live
Anyway Lauren asks the burning question - how do we regulate hospice to assure quality BUT! don't make regulations (?)
Or what she's really saying is don't keep dumping everything on the nurses, which is a universal complaint and valid - but seriously Lauren of course rules etc will have lots of implications that need to be figured out and whatever else you want they're not going to be "free," especially the way VITAS! dude's handlers need them to be free or as close to zero as possible, divided by 2
You just negotiated against yourself - you were advocating for something then immediately advocated against it with the other side's own argument
Anyway, Ira droned on and on about three great policy recommendations from some in-group but after he ran out of breath and stopped talking we still have no idea what these great things are in even the most general sense, which at this point we can all just chuckle and say oh Ira... and move on
Eric tosses out another fat slow juicy grapefruit of a pitch to VITAS! dude - hey so I don't suppose you and your bosses like regulations all that much do you?
And with a mighty swing VITAS! dude smashes a really slow roller down the first base line until it stops at about halfway no he thinks self-regulation is definitely the way to go, then he and Ira fist pump and hug because it's all about quality
Then there's quibbling and second guessing and more negotiating against themselves in an incoherent mess until at one point Eric brings up amyloid eaters the Alz Assoc/pharma scam - and since he's a bright guy of course he sees the connection and the irony of it all before he says let's not bring that up (which was Ira's point a moment ago that the orgs just don't even want to talk about these topics let alone look at them with a critical eye and basic understanding of financial concepts (making money with money)
Then I stopped watching at about 34:00 - thanks, until next time
Tuesday, April 4, 2023
UPDATED! Updated Game Over Update
Rare shot of Ira with mouth closed
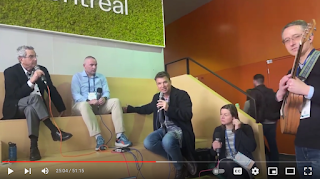
Today I celebrated the halfway point of my journey to listen and annotate the GeriPal podcast video talkapalooza from Montreal - this is not a trip for the fainthearted, especially when it comes to air
It's not that the air gets thinner with altitude - it's the combination of naivety, bullshit, willful ignorance and detached indifference
Sure, this is a 'professional conference' so the voices of patients and families are notably absent...
Which is the whole freaking problem with the same old models we see here, so as long as y'all keep doing this please don't expect anything different, and none of us should expect y'all to find a way through this mess with the same old models
You can check out all of my comments at YouTube, here are today's annotations -
April 4 - OK today I was able to tolerate 2-3 more minutes plus some rewind of Ira's waxing poetic about how great things used to be when the for-profit owners were satisfied with "reasonable" ROI (reasonable to who?) operating "efficiently" (we'll hear that one again) which sounds nice when you're talking about an assembly line but we're talking about patients and families facing serious illness and end of life - oh, wait
Ira wraps up his monologue with the insistence that "our field has a role to play," and probably means himself more than anything because someone so un-self-aware isn't going to realize it's time to STFD and STFU
Eric steps up again and before you know it launches into an upbeat commercial for VITAS, and the punchline is a physician even cleaned the house! he's never seen another hospice do THAT before!!!
So Eric there's this role in the IDT called 'hospice aide' where a person goes into the home and provides personal care including light housekeeping and meal preparation if that's part of the individualized plan of care - check it out (warning - irony ahead)
Anyway after stepping all over what should have been his main question to VITAS dude (what do YOU think of the tension (conflict) between 'excellent hospice care' and 'making lots of money, as much as possible but always more than last time') ...
VITAS dude takes a swing - and there's a slow roller to third, it's not a bunt just really weak contact
Something something Chicago (economics?), then he's in Florida to join a parent facing serious illness
Now he reports to the CEO and is held to metrics so of course he always asks what's best? (for?)
Then he name drops RacistHPNA Board Member Ab '6-Pac' Brody and I'm not sure if he's talking about having or not having an EMR, something about paper and pharmacy and knowing everything and VITAS is great (gonna start writing VITAS!)
Funny story about me and '6-Pac' - he expressed righteous indignation as RacistHPNA BOD member when y'all announced plans to hold in-person in pandemic in freaking Nashville Tenne-freaking-See racist homophobic transphobic Confederate hotbed and thus a risky unsafe place for big swaths of memberships (well, not so big really), and I responded nah - y'all will be there because commerce and careers are more important than caring
How did he respond to that? Let's just say you don't have to be a cishet abled white woman to be a brittle white feminist - in a world of problematic nursing orgs RacistHPNA pretty much heads the list
Anyway VITAS! dude's main point is that his factories are the best - he and Ira high-five chest bump yell 'EFFICIENT!!' - and the only question he asks himself every morning is how many terminally ill people can he help today? HOW MANY?! don't forget he reports to the CEO who reports to the BOD etc
QUANTITY is the only thing that really matters - comps, same store sales - get them to sign on the line that is dotted because even if we have to send a physician over to clean the toilets we'll do whatever it takes, we don't make money on every admission but when you have lots and lots of admissions you can make lots and lots of money
That's the simplest most uncomplicated part of this whole thang
Peace out until next time
Thursday, March 30, 2023
Updated Game Over Updated
Don't piss off the puppeteers
Time to throw this baby out
So I've been slowly making my way through this podcast, because like any good journal article there's a reason (need?) to stop at about every 6th word - either to check out a footnote that turns into a multi-day rabbit hole, think about what you just read and read it again, or just mutter quietly WTAF?
Anyway, the only thing I can manage today is to reflect back on a phrase VITAS dude leaned into right out of the gate - "tax status"
****
I just remembered something VITAS dude said in his first 10 seconds of the podcast - "tax status" - that's an important rhetorical misdirection on his part even if clumsy shallow Weaselspeak
Sure, one difference between not-for-profit and for-profit hospices is that the not-for-profit hospices are exempt from paying the IRS because they're recognized as charitable entities, like your favorite local church
They have to state their case and show evidence - most notably by filing IRS Form 990 every year to report on their finances and operations, including how much the highest earners get paid
It's all very transparent - orgs have to make their filings open and available for public inspection, and legit orgs like Doctors Without Borders and Partners in Health make theirs available right from their websites
For whatever reason I haven't found any hospices that do the same, but online resources like Guidestar provide access independent of the orgs - though they may not be too recent
Plenty of non-profit hospices have reason to be hinky about their finances (exec comp and bonuses in particular), but at least with a little digging it's possible to get some idea
Here's the problem with VITAS dude's memorized propaganda - if the issue is simply one of "tax status," can you seriously imagine this conversion between VITAS godfather Don Gaetz (yeah, he's the dad) and his financial backers in 1984 when non-profit Hospice Care, Inc. became for-profit Hospice Care, Inc:
Don Don - We haven't been paying taxes since 1978, even though we've done a ton of business and now we're looking at even more business paid for by the federal government, the freaking sky is the limit!
Financial Rapscallions (in unison) - What should we do, Don Don?
Don Don - We should definitely start paying taxes!
.
.
.
Financial Rapscallions (in unison) - What a great idea, Don Don!! Yes, let's start paying taxes!!!
You guys crack me up. Please push back on the nonsense, it's literally the least you can do.
Note - I have deep respect for the GeriPal dudes that goes all the way back to the early days of blogging about this stuff, and even wrote a thang for them back in the day, as well as a thang about their thang in tribute
I'm glad they did this podcast, and also very sad because it shows how bleak the future of hospice is
Imagine yourselves as energetic go-getters from Toys R Us completely convinced that those dudes at Bain Capital will have a complete change of heart once they listen to what you have to say
Subscribe to:
Posts (Atom)